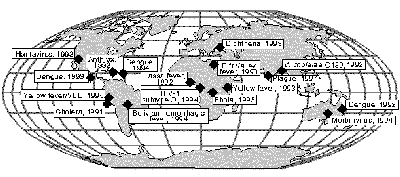
Global Microbial Threats in the 1990s

Forward-looking, sustained efforts to control and ultimately prevent major disease threats form the essential foundation for any plan to successfully address new and re-emerging diseases. The process of responding to international microbial threats encompasses a multitude of activities, including diagnosis of the disease; research to understand its modes of transmission; research to develop adequate means to treat it or prevent its spread; and production and dissemination of the necessary drugs and vaccines. Effective response to outbreaks of infectious disease includes both immediate responses to disease emergencies (discussed in Section II) and on-going activities to develop and maintain the tools to control outbreaks, or, better yet, to predict and/or prevent them before they happen.
Preparation
To be ready to respond effectively to infectious disease outbreaks, whenever and wherever they occur, requires international preparation and planning. The response component of a global infectious disease network must rest on a complex foundation that includes skilled public health workers, national and regional laboratories for diagnosis and research, communications systems, and the commitment of national health ministries. A current goal of WHO is to assist each country to develop its ability to provide laboratory diagnosis of diseases endemic to its area and to refer specimens from suspected newly emergent diseases to an appropriate regional reference laboratory. To reach this goal, each country must train medical workers and laboratory technicians and supply them with appropriate equipment and diagnostic resources.
Several additional international elements must be in place to provide the wherewithal for effective and timely disease control and prevention efforts. First, regional reference laboratories must be maintained to provide diagnostic expertise and distribute diagnostic tests. Second, an international communications mechanism should be made available to receive and analyze global disease surveillance information. Third, regional procedures should be instituted to facilitate the production, procurement, and distribution of medical supplies, including vaccines for disease eradication programs. Fourth, enhanced public education in simple health measures in developing countries must be instituted.
Prevention
Disease prevention is an investment in the young people of the world and in our collective future. Every year, an estimated four million infant and child deaths are prevented by vaccination and other preventive health measures, due to multilateral efforts. The elimination of smallpox would not have been possible without a truly global effort. Similarly, multilateral leadership and resources propel the international program to eradicate polio. Both examples demonstrate the value to American citizens of resources invested in global disease prevention.
In recent years, many countries have dramatically strengthened their health-care delivery systems, even in the face of economic stagnation. Prevention efforts - vaccination, education to change unsafe human behaviors, and other public health measures - are the most cost-effective and beneficial of all measures that address the problem of new and re-emerging infectious diseases. In recent years, a few countries have dramatically strengthened their public health systems even in the face of economic stagnation. However, even these gains are fragile and subject to eclipse by shorter term economic and political pressures.
1. Public health infrastructure in the United States
As a nation, our first-line of defense against infectious diseases is our national system for notifying health authorities of individual cases of infectious diseases. The legal authority for disease reporting rests with the states, which determine which diseases or conditions must be reported by doctors and medical laboratories. In turn, the states voluntarily report cases of more than 40 infectious diseases to CDC. To be effective, our national surveillance system must be comprehensive, including not only reporting and investigation of cases, but also submission of clinical specimens for testing at local, state, or federal public health laboratories. The surveillance system breaks down if any one step - diagnostic testing, case reporting, or follow-up investigation - is not accomplished.
Neglect of the U.S. public health infrastructure
In the past, our national surveillance system for "notifiable" diseases has provided the basis for public health decisions concerning communicable disease prevention and control. However, during the past decade or more, state and local support for infectious disease surveillance has diminished, largely as a result of budget restrictions. In 12 states, for example, no personnel were dedicated to the surveillance of food-borne disease, which is believed to be on the rise (see "Food-borne and Waterborne Infectious Diseases"). In addition, the notifiable disease surveillance system is understaffed in many states. As a result, many of the currently reportable diseases are in fact significantly underreported, and in many areas there is limited followup of the cases that are reported. Moreover, public health agencies are reluctant to add new diseases to the list of notifiable diseases because their capacity to support the surveillance system is already limited by lack of funds and personnel.
Because of this breakdown, targeted federal programs concerned with AIDS, TB, sexually transmitted diseases, and vaccine-preventable childhood diseases have been unable to rely on data from our crippled surveillance network and have developed independent, federally supported parallel surveillance systems to obtain data for their prevention and control activities. Thus, at the same time that AIDS surveillance was being established, other parts of the surveillance system for communicable diseases were failing. A 1993 nationwide survey of public health agencies revealed that -- except for the targeted disease programs noted above -- only skeletal surveillance staff exist in many state and local health departments. At the current level of disease surveillance, it may take hundreds of cases before an outbreak of a non-targeted disease in a large urban area will be detected.
In 1993, a municipal water supply contaminated with the intestinal parasite Cryptosporidium caused the largest recognized outbreak of waterborne illness in the history of the United States. Over 400,000 people in Milwaukee, Wisconsin, had prolonged diarrhea, and approximately 4,400 were hospitalized. Also in 1993, hamburgers contaminated with the bacteria E. coli 0157:H7 and served at a fast-food restaurant chain caused a multistate outbreak of bloody diarrhea and serious kidney disease. More than 600 people got sick; 56 people had kidney failure, and 4 children died. Other outbreaks of food-borne illness in recent years have included cholera from coconut milk from Thailand, Shigella diarrhea linked to green onions from Mexico, and Salmonella diarrhea from an Israeli snack food. These diseases were emerging at the same time that domestic surveillance of infectious diseases was diminishing. A number of factors were associated with the occurrence of the outbreaks of E. coli 0157:H7 and Cryptosporidium. However, the lack of prompt diagnosis and reporting likely contributed to morbidity, mortality, and economic costs.
Three ways to improve domestic surveillance of infectious diseases
1. Strengthen the national notifiable disease system.
For acute infectious diseases that require prompt reporting and investigation of every case (such as botulism and meningococcal meningitis), a national notifiable system works best. Local health departments must be made stronger and more flexible, so that disease-reporting can be modified to include new illnesses as they arise. State, local, and federal public health offices must work in partnership to achieve these goals.
2. Establish sentinel surveillance networks.
For many other diseases, reporting of all cases is unnecessary. Instead, sentinel networks linking groups of health care providers and laboratories to a central data processing center may be particularly helpful in observing rises in the incidence of particular diseases. For instance, such networks can be used to monitor unexplained adult respiratory distress syndrome and childhood illnesses characterized by fever and rash. A good example of a sentinel network is the one established for influenza (see "Sentinel Surveillance for Influenza").
3. Establish public health centers for emerging diseases to prevent future AIDS-like epidemics in the United States.
A different type of sentinel system is required to detect and investigate newly emergent diseases, which by definition are not on any reportable list. A sentinel system for this purpose would perform comprehensive surveillance within several well-defined sites that offer access to various population groups. Such centers could be developed through cooperative agreements with local and state health departments in collaboration with local academic institutions and other governmental or private-sector organizations. Strategically located epidemiology and prevention centers for emerging infections could also be used to monitor antimicrobial drug resistance, foodborne diseases, and opportunistic infections. Each center would conduct population-based surveillance projects, evaluate new diagnostic tests, and implement pilot projects for disease prevention and intervention.
The influenza sentinel surveillance network was established through the American Academy of Family Physicians and includes approximately 150 primary care physicians located throughout the United States. These physicians submit weekly reports of the number of patients seen with influenza-like illnesses by age group, per number of patent visits, as well as the number of hospitalizations among patients with influenza-like illness. A subgroup also collects nasopharyngeal specimens that are sent to a central laboratory for influenza virus identification.
The international component of influenza surveillance involves a network of collaborating laboratories, established in 1947, which now includes over 100 WHO National Collaborating Laboratories. The primary purpose of the network is to detect the emergence and spread of new strains of influenza that may signal a need to update the strains contained in the influenza vaccine. To augment the WHO network, CDC supports a surveillance system for influenza virus isolation at six sites in China, where many pandemic and epidemic strains have first appeared.
2. Public health infrastructure in other nations
The United States is usually informed about disease outbreaks in other countries because we are widely respected as the world's foremost authority on infectious disease recognition and control. Individuals, laboratories, and ministries of health seek to collaborate with CDC, either formally or informally, when they are confronted with an infectious disease problem that they cannot resolve. To ensure that we continue to be notified, we must ensure that we remain ready to assist in national capacity building for disease surveillance, and to respond when asked for assistance.
The effectiveness of a global disease surveillance and response system depends on each nation's capacity to detect and control infectious diseases. Some industrialized countries have become sufficiently concerned about the resurgence of infectious diseases to devote substantial resources to a surveillance effort. In addition, the Executive Board of the World Health Assembly recently passed a resolution that focuses on capacity building related to emerging infectious diseases.
In many developing countries, however, health resources are extremely scarce, and U.S. health experts agree that WHO has not been able to fill the existing gaps in global surveillance and response. Furthermore, major U.S. funding for this purpose is not a likely prospect during this period of federal deficit reduction and downsizing. However, there are several inexpensive, cost-effective actions that can and should be taken.
First, we can encourage and assist other countries to make disease prevention, surveillance, and preparedness a national priority.
Second, we can build new efforts onto long- standing programs and relationships that help other countries to strengthen disease prevention efforts and preparedness by improving their public health infrastructures such as their systems for treating waste water and disinfecting drinking water.
Third, we can identify and preserve existing projects that enhance other countries' capacities to detect and control infectious diseases.
The goal of enhancing other nations' capabilities to monitor and control infectious diseases is in accord with the security and foreign policy aims of the United States. In the post-cold war period, a major objective of U.S. foreign policy is the promotion of sustainable economic development around the globe. Helping other countries to help themselves - to improve the lives of their citizens, develop their economies, and find niches in the global economy - is a major guide for U.S. foreign assistance and aid. Support for international health initiatives is a valuable part of the U.S. effort to promote economic development and political stability.
The U.S. Government's role in international prevention and
control efforts
As mentioned above, the U.S. Government has contributed money, time, and expertise to the successful effort to eradicate smallpox and to the continuing effort to eradicate polio and other childhood diseases. This was accomplished through a sustained interagency and private sector effort. Many or most of the vaccines used in the disease eradication programs were developed in the United States, building on many years of basic research by American scientists.
Many other U.S. Government activities assist developing countries to lay the foundation for effective disease prevention and control, surveillance and response. Most of these programs are supported and organized by USAID, which is the U.S. agency responsible for international sustainable development, humanitarian assistance, and disaster response. Disease control efforts are often thwarted and microbes given fertile breeding grounds by political and economic instability and civil strife. Worldwide efforts to promote good governance, economic development and resolution of conflicts are not out of place in a discussion of how to deal with new and re-emerging diseases. To neglect such efforts is to potentially doom us to costly crisis response making long-term prevention and control difficult or impossible. Thus, activities targeted at improving less developed countries" abilities to conduct surveillance, prevent and control diseases, and prepare for epidemics are integral to sustainable development efforts.
Several specific activities supported by USAID and other U.S. agencies are described in boxes in this section. The overall objectives of these activities are:
The International Center for Diarrheal Disease Research, Bangladesh (ICDDR,B; now known as the Centre for Health and Population Research), is a leading international health research institute in the developing world. USAID has supported the ICDDR,B for over 25 years, dating back to the landmark clinical trials of oral rehydration therapy for cholera. Other scientific achievements include the characterization of new cholera strains; the demonstration of cholera vaccine efficacy in field trials; the development of inexpensive, simple diagnostics for diarrheal diseases; and the development of successful integrated family planning and health services delivery programs through operations research. The ICDDR,B also provides training to scientists from around the world and essential medical care for thousands of Bangladeshis. The ICDDR,B has also provided technical assistance to humanitarian relief efforts in Peru, Zaire, and Rwanda.
Although the United States made the initial investments, the success of the ICDDR/B over the years has attracted multi-donor support from the governments of Switzerland, Canada, and Japan; from multilateral organizations such as the UNDP, the WHO, and UNICEF; and from private foundations such as the Sasakawa and Ford Foundations.
The Applied Diarrheal Disease Research (ADDR) Project, developed by USAID and the Harvard Institute for International Development, has pioneered research capacity building through innovative workshops, consultancies, and research grants. ADDR provides assistance in proposal development and implementation, data collection and analysis in developing countries. ADDR works with collaborating groups of local scientists and policy makers (an effective combination for policy change) to set the research agenda and to develop national networks of investigators. ADDR-sponsored research, which emphasizes social science research, provides new health interventions, better tools for epidemiologic studies, and better case management in priority countries. All of the research is conducted in developing countries.
ADDR has developed a network in 12 developing countries of over 300 scientists who are collaborating successfully in the search for new ways to prevent and control infectious disease outbreaks. The ADDR network in Mexico, for example, is demonstrating how one developing country can slow the evolution of antibiotic resistant microorganisms through appropriate antibiotic prescribing and compliance practices. In an initial study, ADDR scientists determined that educational and managerial interventions in a Mexican Social Security (IMSS) clinic significantly reduced the proportion of children who received antibiotics and anti-diarrheal drugs, and increased the use of oral rehydration therapy. These changes have lasted more than 18 months after the intervention ended. Medication compliance improved among patients in the intervention group even though improving such compliance was not an explicit objective of the intervention.
A second study undertaken by the IMSS extended the same methods to 17 clinics from both the IMSS and the Mexican Ministry of Health, and looked both at diarrheal and acute respiratory diseases. Results from this randomized controlled trial of clinics were very successful; medication costs decreased by 36% and medication waste due to noncompliance and over-prescribing decreased by 51%. Mexico's Minister of Health took an active interest in the studies and, as a result, the IMSS is now implementing a new diarrheal disease treatment program in 12 Mexican states. If successful, this large scale intervention may lessen the likelihood that antibiotic resistant microorganisms will emerge from Mexico.
Saving money and lives through immunization programs.
The success of the effort to immunize children throughout the world against common childhood diseases is dependent on the availability and quality of local immunization programs. Yet limited health budgets in many developing countries limit the number of children who are immunized. USAID has invested in identifying and developing cost-effective technical solutions that save money - and lives.
For example, with USAID assistance, the Program for Appropriate Technology in Health (PATH), has worked with a U.S. company to develop simple monitors for individual vaccine vials that indicate when a vaccine has been exposed to heat and needs to be discarded. Previously many vials were discarded unnecessarily. As much as $20 million will be saved each year on oral polio vaccine alone, a savings that can be used by countries to purchase more vaccine and immunize a far greater number of children.
Diagnostics: Rapid and simple for surveillance and prevention.
Rapid, easy to use diagnostic tests can be invaluable to track the spread of emerging infectious diseases. In the developing world, the capacity to locally manufacture high quality diagnostics has lagged behind pharmaceutical and vaccine production. Yet diagnostic tests manufactured in industrialized countries are often inappropriate for use in developing country health programs. They are too costly, too complex to use, or need supporting laboratory equipment and highly trained technicians. Through its agreement with PATH under the HealthTech Project, USAID has supported the development of a generic low-cost, rapid "dipstick" technology that is suitable for use under field conditions. The dipstick technology is currently used to detect antibodies to HIV-1,HIV-2, and hepatitis B viruses in blood samples, and shows extremely high sensitivity and specificity. The basic technology can be adapted to allow detection of other important diseases.
None of these disease prevention technologies were of interest to the commercial sector initially because they were primarily designed for developing country needs. By advancing the technology, USAID and PATH have been able to stimulate commercial sector interest and investment so that U.S. industry now is producing new products that directly contribute to slowing the spread of diseases in the developing world.
Comprehensive country-level objectives for capacity building have been concisely described by WHO in its January 12-13, 1995 report on emerging infectious diseases.
Regional-level Objectives
Regional-level objectives recommended by U.S. agencies include
Implementation of the recommendations for establishing regional surveillance and response networks will provide significant steps toward the fulfillment of the first three regional level objectives.
Four Target Areas for Capacity Building
Capacity building in support of a national surveillance and response system encompasses a complex set of skills and resources, many of which are readily available in industrialized countries but not in underdeveloped ones. The components of a public health infrastructure include human resources, physical resources, systems for laboratory referral and information exchange, and a favorable policy environment to encourage disease surveillance and permit disease reporting and cooperation with other countries. Recognizing, reporting, and responding to new disease threats involves each of these target areas.
1. Human resources for capacity building
Both categories require people who are trained in the operation, quality control, and maintenance of the equipment.
3. National systems for disease reporting
4. Building a policy environment conducive to participation in a global system
When a serious disease outbreak is suspected, the political authorities of a given nation may be reluctant to report it, fearing loss of trade and/or tourism, or to seek technical assistance for the epidemiologic and laboratory investigation. In the past, this reluctance has had serious consequences. In many cases, diseases have spread unchecked. In some other cases, in which an outbreak was quickly brought under control, unnecessary restrictive measures were imposed by other countries, causing economic damage. Governments should encourage international communication among scientists and public health personnel regarding emerging infectious diseases and request international assistance through WHO when disease outbreaks occurs or when unusual infections are suspected.
Since 1980, the Field Epidemiology Training Programs (FETPs) have set the standard for training in applied epidemiology in many countries. Sponsorship of these programs has given CDC the opportunity to help strengthen the international public health network while reducing the risk that infectious diseases will be imported into the United States.
CDC established the first FETP in Thailand in collaboration with WHO and the Thai Ministry of Health, in answer to a Government of Thailand request for assistance in training in applied epidemiology. Since then, programs have been initiated in 14 countries including Australia, Colombia, Egypt, Hungary, Indonesia, Italy, Mexico, Peru, Philippines, Saudi Arabia, Spain, Taiwan, Uganda, and Zimbabwe. Programs are currently under development in South Africa and the Dominican Republic, and several additional programs are in the preliminary planning stages.
The FETPs are modeled on CDC's domestic Epidemic Intelligence Service (EIS), 2-year training course in applied epidemiology. The FETPs maintain the basic structure of EIS with modifications to suit the needs of the individual host country. The objectives of the program are to:
FETPs directly benefit the countries in which they operate and also provide public health partnership benefits to the United States. Empowering national programs to deal effectively with their own disease control and prevention problems diminishes the need for further direct U.S. involvement. Moreover, working with FETP colleagues throughout the world has yielded a wealth of experience, professional collaborations, and international infectious diseases surveillance connections. For example, because of CDC's participation in Peru's FETP, CDC staff were in place in 1991 to help control the first cholera epidemic in the Western Hemisphere in the 20th century.
During 1981-1993, USAID supported the Africa Child Survival Initiative, Combating Childhood Communicable Diseases (CCCD) project, which was implemented by CDC in 13 countries in sub-Saharan Africa. At the outset the CCCD project, epidemiologic surveillance systems remained fairly rudimentary, despite the advances that the smallpox eradication program had made in the region. There were few epidemiologists, minimal data management capabilities, and few programs that made use of current health data. The CCCD project developed health surveillance programs in a variety of Francophone and Anglophone countries. These included a national program for sentinel infectious diseases surveillance in Zaire; a hospital-based malaria surveillance project in Kinshasa, Zaire; and surveillance of resistance to antimalarial drugs in Guinea, Nigeria, Togo, and Zaire. Several valuable lessons were learned from these projects.
International Clinical Epidemiology Units (INCLEN): The Essential
Role of Training and Research in Surveillance and Prevention of
Infectious Diseases
In 1980 a group of health specialists from the Rockefeller
Foundation, concerned about the growing crisis in global health
care, created INCLEN, a non-profit international program to train
faculty from medical schools in developing nations in clinical
epidemiology. Such training enables medical practitioners to
evaluate the availability, effectiveness and efficacy of
health-care practices in their home countries. In addition, the
physician/epidemiologists extend their vision beyond the
individual patient or hospital ward to better understand the
total impact of disease on the public and the country (medical,
personal, cultural, economic, etc.) and the importance of
prevention strategies.
The multiplier effect of this training program is impressive. It started with five training centers in five countries, and has now (15 years later) trained more than 300 physicians, social scientists, and biostatisticians, who have formed adjunct units in over 40 medical schools in 16 developing countries. These INCLEN units form the backbone of an active research and surveillance network which attempts to identify and confront infectious diseases before they become unmanageable, costly crises. The physician/epidemiologists conduct high-quality research on critical topics such as the economic implications of clinical decisions, cultural factors influencing attitudes and practices toward sickness and health.
USAID supports seven INCLEN units in India. Recently, these units in India collaborated to study the bacterial agent most commonly associated with pneumonia in various locations throughout the country. This activity was built upon the surveillance and treatment capacities established by the INCLEN epidemiology training and research development program. The study showed the pneumococcal pneumonia, treatable with penicillin, was by far the most common cause of pneumonia in Indian children throughout the country. This finding changed the focus of vaccine development and caused the Ministry of health to change its policy for case management of pneumonia which had previously relied on expensive broad spectrum antibiotics rather than the far cheaper and readily available penicillin.
The INCLEN approach demonstrated that use of public health tools (including surveillance of disease patterns and research on the effect of drug treatment) coupled with health economic analyses can lead to efficient and cost-effective preventive and curative interventions.
Emerging vector-borne diseases are a serious problem in Nepal and surrounding countries, posing a continuous threat to maternal/child survival and economic development. For example, the Terai region in southern Nepal has been the focus of a pandemic of Kala-azar (visceral leishmaniasis), which has spread from neighboring areas of India and Bangladesh. This parasitic disease, spread by the bite of an infected sandfly, is rapidly fatal if undiagnosed and untreated and the available chemotherapeutic treatment is costly and losing its' effectiveness. It is estimated that more than 1 million children and adults have been affected in this region alone since the mid-1980s. Sporadic but increasing outbreaks of another emerging disease, Japanese encephalitis (JE), also causes many deaths. Adequate diagnosis and treatment are lacking. Although a preventive vaccine for JE is available, significant cost reductions will be needed if it is to be made affordable for developing countries.
Over the past 40 years, USAID supported the control of malaria in Nepal, and move recently supported the development of a Vector-borne Disease Center for the Division of Epidemiology and Disease Control of the Ministry of Health (MOH) of Nepal. The Center is centrally located in the Terai region where the bulk of vector-borne diseases are found. Through its Environmental Health Project (EHP), USAID provided overall leadership and coordination of a multi-agency response to emerging vector-borne disease in Nepal. In addition, the Government of Japan agreed to provide funding for local use of insecticides in areas in which Kala-azar is endemic. Finally, CDC is providing support for technical training of key staff in surveillance and control methods for JE.
This leveraging of the resources of collaborating agencies and governments has proven to be an essential component in addressing emerging diseases as public health issues, and should be a prerequisite for mounting effective response strategies in the future. The Center in Nepal has also benefited from the environmental health approach of EHP as it plans to conduct operational research to improve understanding of the mechanisms of the diseases at the community level.
As a result of local commitment, hard work, and foreign aid, Nepal will have the local capacity and appropriate tools to monitor future outbreaks of these and other emerging/re-emerging regional vector-borne diseases including malaria, dengue hemorrhagic fever, and plague.
Food and Agriculture Organization (FAO) Reference Centres
French Scientific Research institute (e.g., Senegal, Congo, Cote d'Ivoire)
Pasteur Institutes (e.g., in Algeria, Central African Republic, French Guiana, Iran, Madagascar, Morocco, New Caledonia, Senegal, Vietnam)
Research Institute for Tropical Medicine, Philippines
Institute of Medical Research, Papua, New Guinea
Noguchi Center, Ghana
What made the difference?
Between 1985 and 1991 USAID supported several epidemiologic surveillance systems and child survival programs, including diarrheal disease control programs involving oral rehydration therapy. Education in the use of diarrheal disease control measures, combined with a high level of political and technical coordination, made it possible to deal successfully with cholera when it re-emerged, after an absence of almost 100 years. As cholera spread in Peru, deaths were kept to a minimum through the aggressive use of diarrheal control measures. Such measures were already institutionalized in the public health infrastructure by the Ministry of Health.
A U.S. Government interagency effort (USAID, EPA, DOD, CDC and the FDA) assisted the Government of Peru in responding to the outbreak. Disease control was established in a relatively short period of time because of the programs already in place, including the human and institutional resources developed over time to address diarrheal diseases.
What more can be done to prepare and prevent emerging infectious diseases?
Cholera is spread when food and drinking water are contaminated with fecal waste. The first line in prevention, therefore, is adequate human waste disposal, clean drinking water, and sanitary preparation and storage of food. The technologies necessary to prevent contamination can be as simple and cheap as appropriately placed and maintained latrines, household disinfection of drinking water and frequent hand-washing. Thus education programs in simple but effective interventions may help minimize the potential for future cholera outbreaks.
New technologies and research may also contribute to preparing for and preventing future outbreaks. Research is being conducted to develop a more effective cholera vaccine and to identify useful forecasting tools. The expertise of such institutions as the Center for Health and Population Research is being tapped to provide guidelines and training for NGOs involved in responding to outbreaks of cholera and other diarrheal diseases.
 Return to CISET Report Home Page
Return to CISET Report Home Page